With the release of vaccines in the U.S., many are asking who gets them and when. One of the factors included by policymakers on who needs the decision first is a mortality risk calculator developed by researchers at Johns Hopkins in Baltimore. It measures the mortality of an individual, in the event of infection.
Your own risk is good information to have, as it gives a good indication of personal risk you take when choosing to interact with the outside world. In this article, we have provided for you, a link to the the Johns Hopkins The Mortality Risk Calculator that calculates risk of mortality from COVID-19 in currently uninfected individuals based on input on a set of risk-factors, and community-level pandemic dynamics in the state of residence.
Click on the link below to measure your own risk.

As always, we encourage individuals to use this information wisely. This virus, while constantly being researched, is relatively new- hence the term “novel coronavirus”. The long-term affects that are being seen even in what appeared initially to be minor cases of infection, in what is being called “Post Covid-19 Syndrome”.
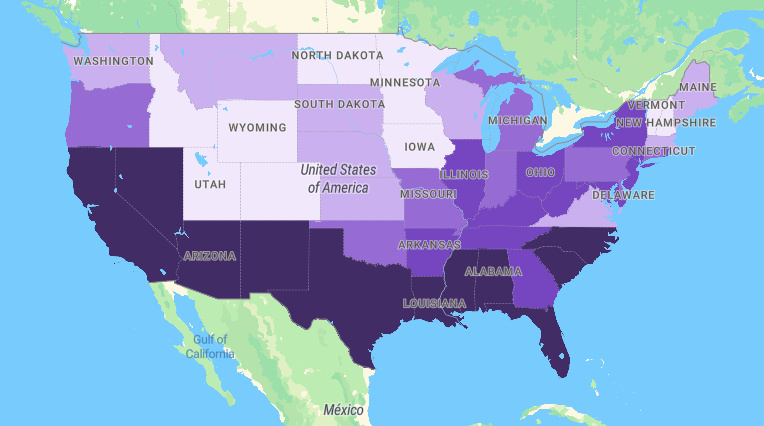
In addition to the individual risk of mortality measured in the calculator, and Interactive Map developed by Johns Hopkins Public Health and University of Maryland researchers in partnership with “PolicyMap” is another of the tools being used by policy makers in deciding to who and where to distribute vaccines. According to Johns Hopkins:
“Researchers at the Johns Hopkins Bloomberg School of Public Health and the University of Maryland created a statistical model of how likely an adult (age 18+) is to die of COVID-19 as compared to the national average, based on demographic information and underlying health conditions. The researchers developed the model based on two sources of information: (1) multivariate-adjusted estimate of risk associated with gender, social deprivation index and 12 pre-existing conditions from the recently published UK-based OpenSAFELY study, and (2) death rates associated with different age and racial/ethnic groups in the US published by the Centers for Disease Control and Prevention (CDC) after performing external covariate adjustment accounting for the correlation of these factors with other risk factors in the model.
Click Below on the Interactive Map powered by PolicyMap.
We at Curus understand that information drives good decision making. While we cannot always determine what others may do with the information given, our job is to help our members make decisions that will lead to the best health outcomes possible in their situations. As more comes to light, and we see the pandemic proportions of COVID-19 decrease, the long-term affects of infection will become more apparent in Post Covid-19 Syndrome and Post Covid Stress Syndrome. Make sure you subscribe to HealthPoints, if did not receive this in your email, as we bring your more information in upcoming issues.

